- Aktueller Stand elektronischer Patientenakten
- Die Einführung elektronischer Patientenakten in Deutschland
- Die rechtlichen Rahmenbedingungen und Regelungen zur elektronischen Patientenakte
- Heutige technologische Fortschritte
- Hauptvorteile der ePA-Lösungen
- Herausforderungen und Risiken bei der ePA-Erstellung
- Datenschutz und Datensicherheit
- Integration und Interoperabilität verschiedener Systeme und Anbieter
- Elektronische Patientenakten: Kosten für die Entwicklung solcher Software
- Kostenrechtfertigung
- Betrachtung der Vorteile von E-Akten
- Zusammenstellung der ePA-Kosten
- Auswahl der optimalen Bereitstellungsmethode
- Berücksichtigung der Implementierungsinvestitionen
- Beachtung versteckter Kosten
- Erstellung eines umfassenden Budgets
- Finanzierung und Unterstützung
- Fazit
In einer Ära des technologischen Fortschritts spielen elektronische Patientenakten eine entscheidende Rolle bei der Verbesserung ärztlicher Versorgung. Um jedoch ihr volles Potenzial auszuschöpfen, ist ein umfassendes Verständnis der finanziellen Investitionen, die für ihre Entwicklung erforderlich sind, unerlässlich. Wenn wir uns mit den Kosten von Patientenakten befassen, betreten wir eine komplexe Landschaft, die von technologischen Anforderungen und Infrastrukturüberlegungen geprägt ist. In diesem Beitrag werden Ihnen die Experten von Andersen erläutern, welche Vorteile elektronische Patientenakten bieten und welche Investitionen Sie erwarten können, wenn Sie solche Softwarelösungen implementieren möchten.
Aktueller Stand elektronischer Patientenakten
Von den gelblichen Pergamenten im alten Ägypten bis hin zur digitalen Darstellung auf einem Tablet haben sich Krankenakten im Laufe der Zeit stark weiterentwickelt. Sie sind für das heutige Gesundheitswesen unverzichtbar.
Moderne elektronische Akten ermöglichen die Erfassung, Speicherung und Verwaltung von Gesundheitsinformationen von Patienten. Diese Funktionalität kann durch die Integration elektronischer Patientenakten mit anderen Gesundheitsinformationssystemen, Plattformen und Geräten erweitert werden. Durch Krankenakten haben autorisierte klinische Mitarbeiter sofortigen Zugriff auf die Krankengeschichten, Testergebnisse, Termine, Medikamente und andere relevante Daten der Patienten. Dadurch wird die Effizienz verbessert, und die Informationen sind leicht zugänglich.
Die Verwendung solcher Software trägt maßgeblich zu einem reibungslosen Arbeitsablauf in Gesundheitseinrichtungen bei. Sie vereinfacht die Führung klinischer Aufzeichnungen und die Berichterstattung von Informationen. In Kombination mit anderen Lösungen wie Echtzeit-Lokalisierungssystemen und Telemedizin-Apps unterstützt sie das medizinische Personal dabei, die Verfügbarkeit von Stationen und Betten zu verfolgen, klinische Abläufe wie Aufnahmen und Entlassungen durchzuführen, Patienten zu überwachen und ihre Vitalfunktionen zwischen den Besuchen zu kontrollieren, und vieles mehr.
Zusätzlich ermöglichen Patientenportale, die mit der ePA verknüpft sind, den Patienten den jederzeitigen Zugriff auf ihre wichtigen Gesundheitsdaten. Dies ermöglicht es den Menschen, besser informiert über ihren Gesundheitszustand zu sein, da sie einfach auf ihre Laborergebnisse, medizinischen Bilder, Rezepte, Versicherungspläne und mehr zugreifen können. Dadurch können Patienten ihre Medikamente besser einhalten und schneller die Anweisungen ihres Arztes erhalten. Dies fördert eine aktive Teilnahme der Patienten an ihrer eigenen Gesundheitsversorgung und unterstützt sie dabei, wichtige Entscheidungen zu treffen.
Die Einführung elektronischer Patientenakten in Deutschland
Die Einführung elektronischer Krankenakten markiert einen wichtigen Meilenstein für die digitale Transformation des Gesundheitswesens in Deutschland. Seit dem 1. Januar 2021 haben alle gesetzlich Versicherten die Möglichkeit, auf freiwilliger Basis eine ePA von ihrer Krankenkasse zu erhalten. Diese digitale Akte ermöglicht eine umfassende Speicherung von medizinischen Befunden und Informationen aus früheren Untersuchungen und Behandlungen in Arztpraxen und Krankenhäusern.
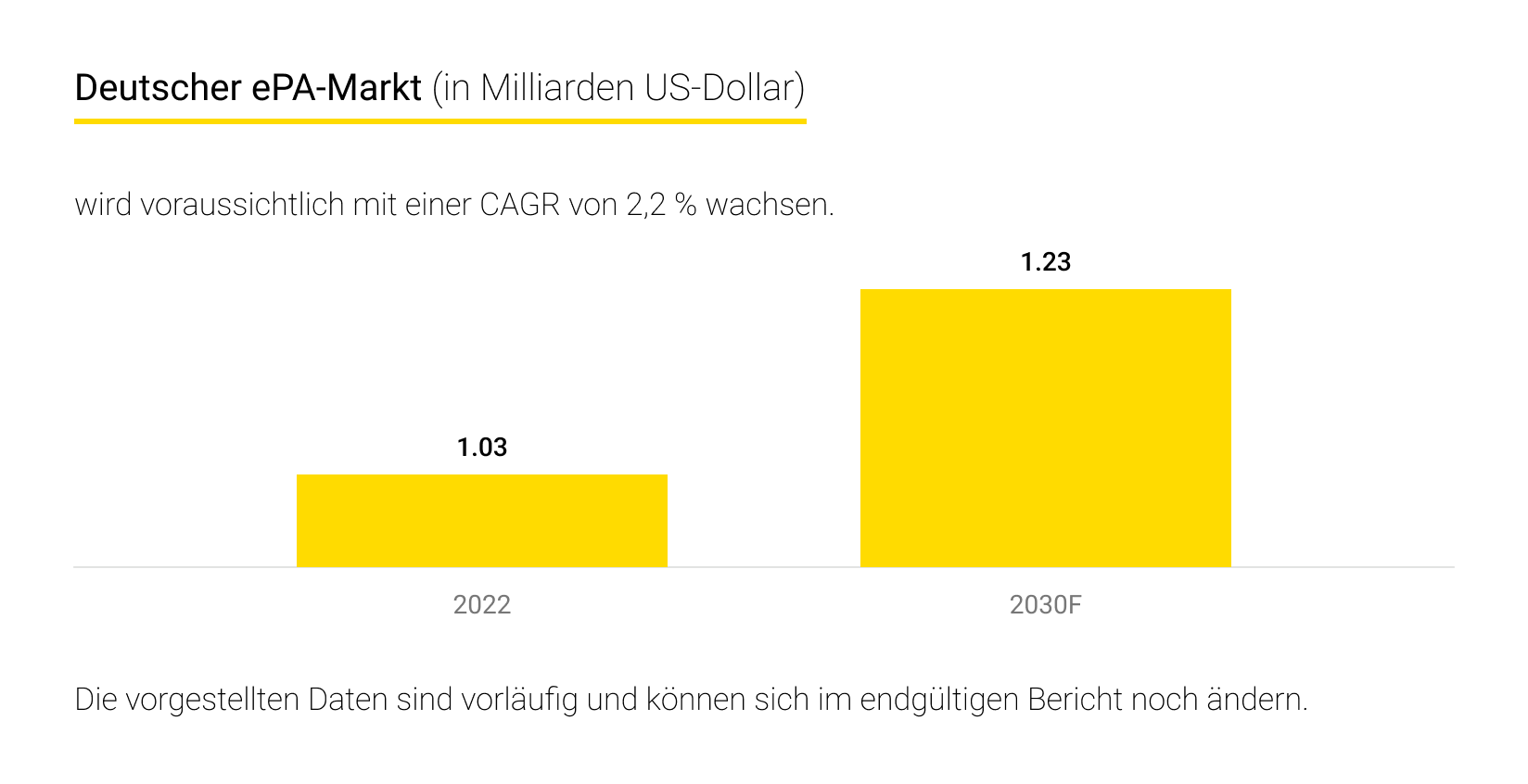
Das Ziel besteht darin, die persönliche medizinische Versorgung zu verbessern, indem leicht zugängliche Daten bereitgestellt werden, Zeit beim Abrufen von Informationen gespart wird und eine gezieltere Patientenversorgung ermöglicht wird. Die Einführung solcher Softwarelösungen stellt somit einen bedeutenden Fortschritt für das Gesundheitswesen in Deutschland dar.
Die rechtlichen Rahmenbedingungen und Regelungen zur elektronischen Patientenakte
Die Bundesregierung unter der Führung von Bundesgesundheitsminister Prof. Karl Lauterbach hat eine umfassende Digitalisierungsstrategie für das Gesundheits- und Pflegewesen eingeführt. Diese Strategie zielt darauf ab, den Datenaustausch aus elektronischen Patientenakten zu erleichtern und den Benutzern die volle Kontrolle über den Zugriff mithilfe einer App zu ermöglichen. Zudem werden pseudonymisierte Daten über das Forschungsdatenzentrum (FDZ) für Forschungszwecke zur Verfügung gestellt.
Durch den rechtlichen Rahmen wird sichergestellt, dass die Entscheidungsgewalt und Kontrolle über Software und die gespeicherten Gesundheitsdaten allein bei den Patienten liegen. Sie haben die Autonomie, über den Umfang der Nutzung, die zu speichernden oder zu löschenden Daten und die Zugriffsberechtigungen für Gesundheitsdienstleister zu entscheiden. Dadurch wird vermieden, dass eine übermäßige Anzahl von Patientenakten erstellt wird, während die Patienten die Kontrolle über ihre Gesundheitsdaten behalten.
Heutige technologische Fortschritte
Die Einführung von ePA-Software in Deutschland hat das Gesundheitswesen revolutioniert. Elektronische Akten schaffen eine reibungslose Verbindung zwischen Versicherten, Gesundheitsdienstleistern, Apotheken und Krankenhäusern und ermöglichen einen mühelosen Informationsaustausch. Dank dieser digitalen Transformation gehören lästige Aufgaben wie die Verwaltung verstreuter medizinischer Dokumente oder die Koordination von Berichten aus verschiedenen Arztpraxen der Vergangenheit an. Sowohl Gesundheitsdienstleister als auch Patienten können jetzt bequem und sicher an einem Ort auf alle erforderlichen Dokumente und Berichte zugreifen. Dies führt nicht nur zu einer Reduzierung von doppelten Untersuchungen, sondern entlastet auch Patienten und medizinisches Fachpersonal von übermäßiger Arbeitsbelastung.
Hauptvorteile der ePA-Lösungen
ONC hat die folgenden Vorteile der ePA-Lösungen im Vergleich zum herkömmlichen Papierdokumenten-Workflow identifiziert:
- Verfügbarkeit von Daten
Die medizinischen Informationen der Patienten sind jederzeit vollständig und leicht zugänglich, was zu einer besseren Koordination und Effizienz in der Versorgung führt.
- Verbesserte und sichere Interaktion und Kommunikation zwischen Patienten und Anbietern
Nur autorisierte Benutzer haben Zugriff auf Patienteninformationen und können diese nutzen und teilen. Patienten erhalten einen verbesserten Zugang zur Gesundheitsversorgung, während Anbieter nahtlos Überweisungen und E-Rezepte erstellen sowie Bilder und Laborergebnisse austauschen können.
- Steigerung der Produktivität der Anbieter durch optimierte klinische Arbeitsabläufe
Digitale Krankenakten ermöglichen eine bessere Planung für Patienten und Personal, vereinfachen die medizinische Kodierung und Abrechnung, verbessern die Work-Life-Balance der Anbieter und senken die Pflegeausgaben.
- Erhöhte Sicherheit für Patienten
Eine genaue Identifizierung der Personen ermöglicht präzisere Medikamentenverschreibungen, reduziert medizinische Fehler und unterstützt die klinische Entscheidungsfindung.
E-Akten haben nicht nur in der alltäglichen Praxis von Krankenhäusern und Zahnkliniken ihre Wirksamkeit gezeigt, sondern haben sich auch während des Ausbruchs von Covid-19 als äußerst nützlich erwiesen, insbesondere bei der raschen Einrichtung temporärer Gesundheitseinrichtungen.
Ein herausragendes Beispiel für ihre Wirksamkeit ist die hohe Impfrate gegen Covid-19 in Israel. Dank eines effektiven Gesundheitsinformationssystems, das 100 % der Anbieter und 100 % der Einwohner des Landes abdeckt, konnten die israelischen Gesundheitsbehörden die Impfpriorisierung effizient festlegen und schnell umsetzen. Dies führte zu einer bemerkenswert schnellen Durchführung der Impfungen.
Herausforderungen und Risiken bei der ePA-Erstellung
Datenschutz und Datensicherheit
Die Gewährleistung eines starken Datenschutzes und die Aufrechterhaltung eines hohen Maßes an Datensicherheit sind entscheidende Herausforderungen. Da vertrauliche Patienteninformationen digital gespeichert und übertragen werden, ist es von größter Bedeutung, diese Daten vor unbefugtem Zugriff und möglichen Verletzungen zu schützen.
Ein zentrales Anliegen besteht darin, die Privatsphäre der Patienten zu schützen. ePA-Lösungen enthalten äußerst persönliche und vertrauliche Informationen wie Krankengeschichte, Diagnosen und Behandlungen. Daher ist es von höchster Wichtigkeit, strenge Sicherheitsmaßnahmen zu implementieren, um unbefugten Zugriff auf diese Daten zu verhindern. Dies erfordert den Einsatz von Verschlüsselungstechniken, sichere Authentifizierungsverfahren und strikte Zugriffskontrollen, um sicherzustellen, dass nur autorisierte Personen Zugriff auf die elektronischen Patientenakten haben.
Darüber hinaus erhöht sich das Risiko von Datenschutzverletzungen, da Softwaresysteme über verschiedene Gesundheitsdienstleister, Apotheken und Krankenhäuser hinweg vernetzt sind. Der Datenaustausch zwischen unterschiedlichen Systemen und Anbietern birgt Schwachstellen, die von bösartigen Akteuren ausgenutzt werden können. Die Gewährleistung einer sicheren Integration und Interoperabilität stellt hierbei eine große Herausforderung dar.
Um diesen Herausforderungen zu begegnen, müssen Entwickler robuste Cybersicherheitsprotokolle etablieren. Dazu gehören regelmäßige Sicherheitsbewertungen, Schwachstellentests und die zeitnahe Behebung aller identifizierten Schwachstellen. Zudem spielen Schulungen und Sensibilisierungsprogramme für Mitarbeiter eine entscheidende Rolle bei der Förderung einer Kultur der Datensicherheit und des Datenschutzes.
Integration und Interoperabilität verschiedener Systeme und Anbieter
Gesundheitsdienstleister nutzen oft verschiedene Softwarelösungen von unterschiedlichen Anbietern. Die reibungslose Kommunikation und der Informationsaustausch zwischen diesen Systemen sind entscheidend für die Effektivität und Effizienz.
Eine große Herausforderung besteht darin, dass es keine standardisierten Datenformate und Protokolle in den verschiedenen Systemen gibt. Jeder Anbieter verwendet möglicherweise eigene Formate, was den Austausch und die Interpretation von Daten zwischen den Systemen erschwert. Dadurch kann es zu mangelnder Interoperabilität und unvollständigen elektronischen Patientenakten kommen.
Die nahtlose Integration von medizinischen Geräten, Wearables und Fernüberwachungssystemen kann die Qualität der Patientenversorgung erheblich verbessern. Allerdings müssen technische und Kompatibilitätsprobleme überwunden werden, um diese Integration zu ermöglichen.

Um diese Herausforderungen anzugehen, ist die Entwicklung und Implementierung von Interoperabilitätsstandards von großer Bedeutung. Durch die Etablierung gemeinsamer Datenformate, Protokolle und Schnittstellen können verschiedene Systeme und Anbieter effektiv miteinander kommunizieren. Dadurch entstehen umfassende und integrierte elektronische Patientenakten, die Gesundheitsdienstleistern fundierte Entscheidungen ermöglichen und eine personalisierte Pflege unterstützen.
Elektronische Patientenakten: Kosten für die Entwicklung solcher Software
Bei der Einführung eines Systems ist es für Gesundheitsorganisationen wichtig, die ePA-Kosten zu verstehen und ein angemessenes Budget festzulegen. Lassen Sie uns verschiedene Faktoren betrachten.
Kostenrechtfertigung
Für viele Gesundheitsorganisationen kann es eine Herausforderung sein, die Investitionen in ein System zu rechtfertigen, insbesondere wenn sie mit geringen Gewinnspannen arbeiten. Allerdings bieten solche Softwarelösungen erhebliche Vorteile, die über die Einhaltung gesetzlicher Vorschriften hinausgehen. Um überzeugende Argumente für die Investition zu liefern, sollten Sie die folgenden Strategien in Betracht ziehen:
- Kosten-Nutzen-Analyse
Stellen Sie die Bereiche in Ihrer Organisation heraus, die von einer Verbesserung profitieren könnten, wie zum Beispiel die Qualität der Pflege, der Kundenservice oder die Effizienz.
- Prognose des Returns on Investment
Präsentieren Sie kurz- und langfristige Prognosen, die verdeutlichen, welchen finanziellen Nutzen die Implementierung des Systems voraussichtlich mit sich bringt.
- Gesamtkosten des Eigentums
Führen Sie eine umfassende Analyse der kurz- und langfristigen Kosten von Patientenakten durch, die mit dem ePA-System verbunden sind, und stellen Sie sicher, dass Entscheidungsträger die finanziellen Auswirkungen verstehen.
Betrachtung der Vorteile von E-Akten
Studien zeigen, dass Praxen die Kosten für die ePA-Implementierung in etwa 2,5 Jahren wieder einspielen können und dabei Netto-Vorteile von rund 23.000 US-Dollar pro Jahr und Vollzeitmitarbeiter erzielen. Die Vorteile erstrecken sich jedoch nicht nur auf finanzielle Gewinne, sondern umfassen auch:
- Steigerung der Effizienz
- Verbesserung der Pflegequalität
- Verringerung von Verschwendung
- Bessere organisatorische und gesellschaftliche Ergebnisse

Zusammenstellung der ePA-Kosten
Die Kostenermittlung für ein System kann aufgrund verschiedener Faktoren wie den benötigten Funktionen, der Bereitstellungsmethode (Cloud oder On-Premise), dem Umfang der Installation und den Hardware-Upgrades eine Herausforderung darstellen. Bei der Berücksichtigung der geschätzten Kosten von ePA sollten Sie Folgendes beachten:
- Durchschnittliches Budget pro Benutzer
Aktuelle Studien deuten darauf hin, dass ein durchschnittliches Budget von 6.000 US-Dollar pro Benutzer angemessen ist. Einzelpraxen geben in der Regel mehr aus als größere Praxen.
- Gesamtbetriebskosten (Total Cost of Ownership, TCO)
Die TCO-Berechnungen ermöglichen eine umfassende Bewertung der kurz- und langfristigen Ausgaben. Die geschätzten TCO für cloudbasierte Systeme belaufen sich durchschnittlich auf 58.000 US-Dollar über fünf Jahre, während On-Premise-Systeme etwa 48.000 US-Dollar betragen.
Gehen Sie auf die folgende Seite, um die Kosten für Ihr individuelles Projekt zu berechnen.
Auswahl der optimalen Bereitstellungsmethode
Die Entscheidung zwischen cloudbasierten und lokalen Bereitstellungsmethoden hat langfristige Auswirkungen auf die Kosten von digitalen Patientenakten. Während cloudbasierte Systeme geringere anfängliche Investitionen aufweisen, müssen Faktoren wie Zuverlässigkeit, zusätzliche Hardwareinvestitionen, Wartung des Systems und Sicherheitsaspekte berücksichtigt werden.
Berücksichtigung der Implementierungsinvestitionen
Die Kosten für elektronische Patientenakten können je nach Kontext und spezifischem Implementierungsplan variieren. In typischen Praxen mit mehreren Ärzten belaufen sich die Ausgaben für die Softwareimplementierung auf etwa 162.000 US-Dollar, wobei 85.500 US-Dollar für Wartungsausgaben im ersten Jahr vorgesehen sind. Die Ausgaben für die Implementierung von Software in Krankenhäusern variieren erheblich, wobei einige Organisationen weniger als 5 Millionen US-Dollar und andere mehr als 20 Millionen US-Dollar investieren.
Beachtung versteckter Kosten
Diese können das Budget beeinflussen. Zu den indirekten Kosten von ePA gehören möglicherweise Einbußen bei den Einnahmen, Produktivitätsverluste und eine geringere Anzahl von Patientenbesuchen während der Implementierungsphase.
Erstellung eines umfassenden Budgets
Beim Erstellen eines Budgets sollten Unsicherheiten und potenzielle Eventualitäten berücksichtigt werden:
- Hardware
Ausgaben in Verbindung mit Servern, Computern, Druckern, Scannern und anderen Peripheriegeräten.
- Software
Ausgaben im Zusammenhang mit Softwarelizenzen, Erweiterungen und Upgrades.
Finanzierung und Unterstützung
Bei der Finanzierung der Entwicklung eines Systems stehen Gesundheitsorganisationen verschiedene Optionen zur Verfügung, um die finanzielle Belastung der Implementierung neuer Software oder der Aktualisierung bestehender Systeme zu verringern. Hier sind einige Möglichkeiten zur Finanzierung zu beachten:
- Öffentliche Fördermittel
Bundes- und Landesregierungen gewähren oft Zuschüsse, um Gesundheitsorganisationen bei der Einführung von Softwaresystemen zu unterstützen. Diese Zuschüsse können regional spezifisch sein oder auf bestimmte Aspekte wie Interoperabilität oder Datensicherheit fokussiert sein.
- Private Stiftungen
Viele private Stiftungen bieten Zuschüsse und Finanzierungsprogramme für Gesundheitsorganisationen an, die Softwarelösungen implementieren oder verbessern möchten. Diese Organisationen priorisieren oft Projekte, die darauf abzielen, die Patientenversorgung, den Datenzugang und die Gesundheitsergebnisse zu verbessern. Durch Recherche und Kontaktaufnahme mit relevanten Stiftungen können bedeutende Finanzierungsmöglichkeiten erschlossen werden.
- Branchenspezifische Förderung
Einige Branchen wie Pharmaunternehmen oder Hersteller medizinischer Geräte bieten möglicherweise Förderprogramme oder Partnerschaften an, um die Entwicklung von Lösungen zu unterstützen. Diese Kooperationen können finanzielle Unterstützung, technisches Fachwissen und Zugang zu Ressourcen bieten, um den Implementierungsprozess zu beschleunigen.
- Lieferantenfinanzierung
IT-Dienstleister können Finanzierungsoptionen wie Ratenzahlungspläne oder Zahlungsaufschubpläne anbieten, um die Einführung ihrer Software zu erleichtern. Durch Gespräche mit den Anbietern über mögliche Finanzierungsvereinbarungen können Gesundheitseinrichtungen die anfallenden Vorlaufkosten für den Kauf oder die Aktualisierung eines Systems bewältigen.
Fazit
Elektronische Patientenakte-Software ist einerseits eine fortschrittliche Technologie, die die medizinische Versorgung verbessern kann, andererseits aber auch eine Herausforderung darstellt. Aspekte wie Datensicherheit, Interoperabilität und Benutzerfreundlichkeit müssen sorgfältig berücksichtigt werden während der Entwicklung. Dennoch kann eine korrekt erstellte und implementierte Software einen großen Beitrag zur Rationalisierung der Prozesse in Gesundheitseinrichtungen leisten und die Effizienz sowie die Qualität der Pflege steigern.
Andersens Entwickler stehen Ihnen zur Verfügung, um maßgeschneiderte Lösungen zu erstellen. Gerne bieten wir Ihnen eine IT-Beratung im Gesundheitswesen an, um die besten Möglichkeiten für Ihr Unternehmen zu besprechen. Kontaktieren Sie uns, um Ihre Krankenakte-Anforderungen und Kosten zu besprechen.













